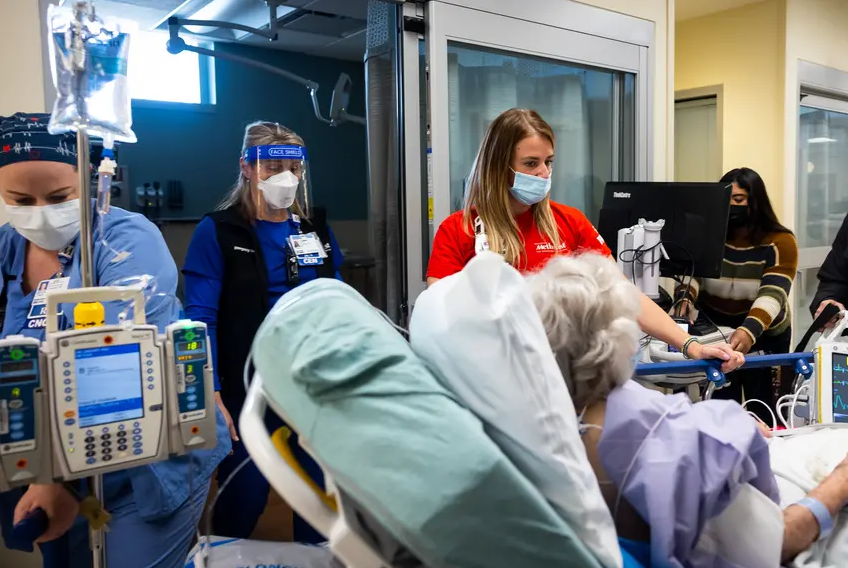
After an anxious January marked by a wave of COVID-19 infections that pushed Texas hospitals and intensive care units to their limits, the number of Texans in the hospital with COVID-19 across the state has been in a steady decline for about a week, according to state health data.
The decrease is the latest in a series of hopeful signs that the surge driven by the highly contagious omicron variant may be starting to abate, forecasters and health officials say.
If the trend continues, the state would have passed its peak hospitalizations for this wave on Jan. 20, when Texas hospitals reported 13,371 patients with COVID-19 — a number that has decreased daily since then. That falls short of the record 14,218 hospitalizations the state saw a year ago on Jan. 11, 2021.
On Monday, the number of Texans in the hospital with COVID-19 was 11,997, the lowest number the state has seen in nearly three weeks. Forecasters and health officials feared last month that hospitalizations could reach new pandemic highs, but now say it’s likely the state won’t reach that mark during this surge.
The decline is a welcome development for doctors, nurses and other officials in the state’s overwhelmed hospitals at the tail end of what, in some areas, was the fifth wave of infections in the past two years.
In the harder-hit metro areas such as Austin and Houston, hospitals reported record-breaking numbers of patients with COVID-19 last month — but the situation is improving.
At Texas Children’s Hospital in Houston, the number of young patients with COVID-19 and the percentage of positive tests in the past six weeks far outpaced any records set during the prior two years, said Dr. James Versalovic, the hospital’s pathologist-in-chief.
Now, positivity rates are down by a third, and the number of patients with COVID-19 is down by about 70%, he said. Those numbers are still higher than records set in the hospital during the delta surge, but they are dropping steadily — albeit slowly, he said.
“We are optimistic. We are breathing a bit more easily this week,” Versalovic said. “We do see light at the end of the tunnel, but it’s a long tunnel. We are looking forward to March.”
Dr. James McCarthy, a chief physician executive and executive vice president for Memorial Hermann Health System in Houston, said in a recent TV interview that the surge appears to be easing up at those facilities.
“We’re feeling very optimistic that we’ve crested this wave,” he said. “We feel like the hospitals have weathered this storm again.”
The state has also seen daily new COVID-19 cases decline by more than a third since last week, as well as a drop in positivity rates. And the number of ICU beds available in the state has started to increase again after it reached its lowest level since the start of the pandemic.
But with more than 25% of tests still coming out positive, the levels of virus still surpass what was seen during the delta surge and “would have been mind-boggling at any point before December,” said Chris Van Deusen, spokesperson for the Texas Department of State Health Services.
“So people should still be cautious,” he said.
Experts also say it’s hard to predict whether another variant may arise that could cause another surge, or how long the natural immunity from an omicron infection might last.
But the downward trend should continue as long as people don’t get too confident too fast, drop their guards and start acting like the pandemic is over, said Anass Bouchnita, a researcher at the University of Texas COVID-19 Modeling Consortium, which uses data and research to project the path of the pandemic.
“All of that is a good sign, but of course it’s not the end,” he said. “We know that around half of the infections and hospitalizations and deaths will occur after the peak, so this is not the finish line. It’s not time to let our guard down. We need to keep up the vigilance.”
That means to get vaccinated but also, he said, to continue masking up, hand-washing and social distancing so the transmission continues to subside.
The number of hospitals reporting full ICUs last week was at 73, still well under the pandemic record of 100 over the summer, and a decrease from the week before.
Still increasing, however, are the daily reported deaths, which don’t usually start declining until a few weeks after hospitalizations peak.
The deadliest wave of the pandemic hit over the holidays in December 2020 and January 2021, just weeks after the vaccine was given emergency use authorization in the United States and very few people had access to it. The numbers of hospitalizations and deaths from COVID-19 hit highs that the state hadn’t seen before and has not seen since.
During the delta wave of last summer, the state put record numbers of children in the hospital with COVID-19 but missed the previous pandemic record for statewide hospitalizations by only a few hundred.
The most recent surge, which started in December, shortly after the omicron variant was detected in Texas, saw case counts and positivity rates in Texas top previous pandemic records, as well as pediatric hospitalizations. The same thing happened nationally.
Compared with the deadlier delta variant surge last September, the most recent wave brought about by the more contagious omicron variant comes with some important caveats, experts say.
Omicron is more easily spread than any of the other versions, taking down vital health employees for days at a time when more people are becoming infected.
Nearly 60% of the state is fully vaccinated, which experts say protects against hospitalization, and the omicron variant itself appears to produce less-serious symptoms than previous iterations. And while treatments are in short supply, there are more approved now than there were during the last surges.
But omicron is still leaving chaos in its wake.
“We’re in a different situation now than we were a year ago,” said Dr. David Lakey, vice chancellor for health affairs and chief medical officer at the University of Texas System, and former state health commissioner. “Having some tools out there, having experience with the virus, having the most vulnerable individuals immunized — that helps a lot. On the other hand, the hospitals have been doing this a long time and they’re very burned out and they’re very short-staffed right now and they are going as hard as they can to care for individuals.”
The good news
ICU admissions for people with COVID are lower than they were during the last peak a year ago, and fewer of those patients need ventilators, according to state data. Smaller percentages of patients who test positive are being admitted into the hospital for COVID treatment, and hospital stays are getting shorter, according to hospital officials.
Those trends signal that the virus is making Texans less sick, overall, which officials hope will not only reduce deaths and suffering but also, eventually, the pressure on hospitals.
“That is a bright spot,” Lakey said.
At the height of the delta surge, more than 100 hospitals in Texas reported that their ICUs were full to capacity. By comparison, at least 73 hospitals reported that their ICUs were full last week.
In Dallas-Fort Worth-area hospitals, even though most of the area’s major hospitals were reporting ICU capacity filled to more than 95%, about half of those patients have COVID-19, similar to the share during delta, said Steve Love, president and CEO of the DFW Hospital Council.
Meanwhile, the number of ICU patients needing ventilators dropped by roughly 50% in the region compared with the other two surges, Love said.
At Houston Methodist The Woodlands Hospital, north of Houston, they’re seeing fewer ICU beds used by COVID patients than they did during the delta surge. But chief medical officer Jason Knight said unvaccinated patients and those with preexisting medical conditions are still at risk.
“With omicron, we’re seeing a lot more people with complex medical problems, where even though the [COVID] infection is mild, it’s pushing them over and causing their complex medical problems to result in ICU admissions and potentially deaths,” he said.
Staffing crunch
The waves of people showing up at Texas hospitals come at a time when the health care industry is experiencing a historic staffing crisis two years into a pandemic that has killed more than 78,000 people in the state.
And while hospital stays are growing shorter, they are still extended in some cases by the lack of nursing home beds available for patients who are in postoperative recovery or need long-term care — a problem exacerbated by staffing shortages at long-term care facilities.
The total number of hospital beds available statewide for all patients is lower than it was when hospitalizations peaked a year ago. That’s due to a combination of staff members and their families being out sick with omicron, nurses leaving for contract work, and employees quitting the industry altogether because of burnout or fears of infection.
At the height of last year’s January surge, the state had some 14,000 medical staffers deployed in the hardest-hit hospitals. During the delta wave last summer, about 8,000 nurses were sent to help.
So far during this surge, the state has contracted with about 4,400 travel nurses for hospitals that need them.
In mid-January at the Golden Plains Community Hospital in the Panhandle town of Borger, nurses were absent in the medical-surgical department as well as the emergency room, the lab and the clinic, while the hospital sees a surge in cases and hospitalizations. Only a third of that county’s residents are vaccinated.
All 10 of the employees who were absent on a recent day last month were out with COVID-19, said CEO Don Bates.
“Every day is a new battle,” Bates wrote in an email. “If it comes to shutting down surgery and pulling nurses from our clinics or OB — which there aren’t many left — we’ll do what we have to do to care for the COVID sick, until we absolutely can’t take any further admissions. Then our docs will have to focus on what the Panhandle Regional Advisory Council has been calling the ‘salvageable.’ …
“Not my words,” he added. By the end of January, Bates was home sick with COVID-19, too.
Nationwide, 81% of ICU capacity is being used, with 29% of those patients diagnosed with COVID-19, according to federal data. Texas ICUs are at a 92% occupancy rate, with about 39% of patients positive for COVID-19.
The influx of omicron cases has created a vicious cycle for many hospitals, where administrators fear that the increased demands on nursing staff may lead to more of them burning out or leaving the profession.
At Houston Methodist The Woodlands Hospital, patients are staying in the emergency department far longer than usual, waiting for a bed to open up.
“We’re trying to take care of essentially an inpatient unit down in our emergency department … in addition to [nurses] trying to do their normal jobs,” said Knight, the chief medical officer there. “A lot of nurses are getting stretched really thin. That’s why a lot of them are getting frustrated. That’s why some people are leaving.”
Knight said the current staffing crunch has created a “competitive environment” for health care, with an increase in frustrated and occasionally rude patients.
The role of vaccination
Prevention protocols such as masking, social distancing and limiting travel play a big role in lowering hospital rates, officials and experts say.
But the big weapon against overwhelming hospitals with severe cases is vaccination, which has been proven highly effective at keeping those who are inoculated out of the hospitals and intensive care units.
About 58% of Texans are fully vaccinated. Nationwide, that number is nearly 63%.
One thing Lakey, the University of Texas System chief medical officer, credits with keeping severe illnesses down and ICU numbers lower than they could be is the high vaccination rate Texas is reporting among its most vulnerable residents ages 65 and older. Some 84% of them have been fully vaccinated.
“The really at-risk individuals of having severe disease, we’ve given them some protection so they’re less likely to go to the ICU and less likely to die because they’ve been immunized,” Lakey said. “You are seeing breakthrough infections, but the vaccines do protect from the severe disease, a significant amount of protection.”
In Montgomery County, where Houston Methodist The Woodlands is based, only 53% of residents are vaccinated, which is the lowest rate for Texas counties with populations exceeding 500,000. Roughly 17% of residents have received booster shots.
Nurses and doctors say that after nearly two years on the front lines, their empathy for the unvaccinated patients who will require their care is diminished.
“The tragedy of COVID is, it’s happening behind the doors of our critical care rooms, in our [ER], in our ICU. … There’s very few people in the community that has ever seen somebody suffocate and die from COVID,” Knight said. “That is totally and completely preventable. I just think that that is incredibly tragic, and that’s hard emotionally on our nurses and it’s hard emotionally on our staff.”
This article was originally posted on Texas COVID-19 hospitalizations down as omicron wave appears to crest